INTRODUCTION
Torticollis is a clinical symptom characterized by a lateral head tilt towards one shoulder with a contralateral chin rotation towards the other. The term comes from the Latin words “tortus” (twisted) and “collum” (neck). This disorder occurs at all ages, from newborns to adults, and can have many underlying causes. Most often, this deformity will be present on the right side, and up to 20% of patients may also have concurrent developmental dysplasia of the hip.1 The most common origin of congenitally occurring torticollis is congenital muscular torticollis (CMT), typically associated with either an imbalance of strength or length of the sternocleidomastoid muscles. Torticollis can also be classified into acquired torticollis, which can present at any time but most often between five and twelve years of age.2 Torticollis is a symptom rather than a diagnosis. As such, there are many etiologies to evaluate regarding the pathogenesis of torticollis, especially when considering age and length of symptom persistence [Figure 1].
The true pathophysiology of CMT is currently unknown, with various theories proposed in the literature.1–17 However, the most common theories suggest unilateral contracture of the sternocleidomastoid, typically causing rotation of the chin to the contralateral shoulder.2,3 Fibrotic changes and shortening are often seen in the sternocleidomastoid. The etiology could be any variety of intrauterine and perinatal events leading to fibrotic shortening, but other developmental causes have been observed, too.
CMT typically responds well to conservative treatment options such as physical therapy, but surgical interventions are occasionally required. There are several surgical options for surgery depending on the indication, ranging from unipolar sternocleidomastoid resection to radical resection.8 Due to the rising incidence of torticollis and craniofacial asymmetries (attributed to the increased use of infant positioning equipment, the Safe to Sleep campaign, and other factors that lead to increased head rest against firm surfaces), awareness of the best practices regarding the prevention and the diagnosis of torticollis is vital.9 Therefore, this review aims to comprehensively evaluate data on the etiology, management, and treatment of torticollis and provide insight into strategies that may improve patient outcomes and care coordination amongst providers.
CONGENITAL TORTICOLLIS
Most commonly, congenital torticollis is due to a persistent contracture in the sternocleidomastoid muscle, a condition known as congenital muscular torticollis (CMT). In a tertiary care center, close to 82% of all children presenting with torticollis were found to have an etiology of CMT.10 CMT is the third most common congenital anomaly after congenital dysplasia of the hip and calcaneovalgus feet.11 There is a worldwide incidence rate of congenital torticollis between 0.3% to 2%,5 but separate studies have shown up to 16%.6 There is a male-to-female ratio 3:2, which often affects the right sternocleidomastoid muscle more than the left, which is a 3:1 ratio.2 CMT is typically identified in neonates and infants within the first month of life but can develop or persist at any time during the initial year of life. It is often unilateral but can be bilateral in rare cases. CMT is typically categorized into three types: (1) Postural torticollis, (2) Muscular torticollis, and (3) Sternocleidomastoid mass.5 In postural torticollis, there is a preferential laterality to the infants’ head positioning and clinical features of torticollis but with no muscle tightness. Conversely, muscular torticollis can show tightness of the sternocleidomastoid muscle and a limited passive range of motion. Finally, sternocleidomastoid mass can present in about 50% of cases with a fibrotic thickening of the sternocleidomastoid muscle that can sometimes be palpable as a fusiform fibrous mass and a limited passive range of motion.11
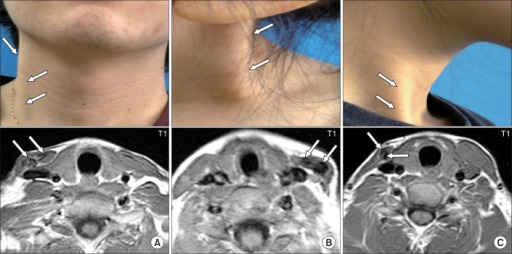
Most studies point toward the pathophysiology of CMT to be due to any combination of birth trauma, prenatal or perinatal compartment syndrome, and intrauterine constraint (oligohydramnios, first-born, breech, etc.) leading to impaired sternocleidomastoid development.12,13 All three of these theoretical etiologies may go hand in hand when discussing the development of CMT. Head positioning in utero can injure the sternocleidomastoid muscle while leading to venous compression and decreased blood supply during muscle development, and shoulder injury during delivery can influence the laterality of the torticollis.1,2,5,11–13 Interestingly, Magnetic Resonance Imaging (MRI) scans of infants with CMT showed increased intensity in the sternocleidomastoid muscle, similar to what is observed in compartment syndrome of other areas in the body.13 This could suggest compression or stretching of the muscle perinatally, leading to injury. Additionally, it has been hypothesized that the swelling within the sternocleidomastoid muscle is due to hematoma formation due to birth trauma, which is then replaced by a fibrous thickening as the hematoma resolves.14 This is supported by histological examination, where the accumulation of fibroblasts can be visualized surrounding degenerative skeletal muscle fibers, leading to muscle atrophy and the accumulation of scar-like collagen. Emerging data has shown that this fibroblastic hyperplasia can lead to increased myocyte apoptosis, endomysial and perimysial fibrosis, and subsequent tightness of the affected muscle.3 It has been shown that the degree of fibrotic change is proportionate to the child’s age at presentation.3
Secondary deformities are often present concurrently with CMT and can be used in diagnosis. As stated previously, there can be concomitant developmental dislocation of the hip (DDH) present in up to 20% of patients with CMT.1 This is high enough to warrant investigation for hip dysplasia when a patient is diagnosed with CMT and vice versa. However, few patients with concomitant CMT and hip dysplasia require further treatment for acetabular dysplasia.15 Factors associated with DDH include pre- and post-natal fetal positioning, genetic factors, oligohydramnios, and breech presentation. These factors parallel those that predispose patients to CMT. Unsurprisingly, deformities associated with birth trauma, such as cranial deformation, brachial plexus injury, and rib cage asymmetry, are all associated with CMT.6,10 Cranial deformations include skull and facial asymmetry: asymmetric ear positioning and mandibular hypoplasia. Interestingly, it has been suggested that mandibular hypoplasia can be present in up to 60% of CMT cases ipsilateral to the affected side and could be useful for early diagnosis.12 Many deformations could be associated with increased labor time, forceps delivery, and larger babies.6 It is unclear if there is a genetic disposition that inclines patients to these deformities. Additionally, foot deformities such as metatarsus adductus and tapiles calceneovalgus have been observed in about 2-3% of CMT patients.16 It has been theorized that increased uterine packing leads to abnormal posture and physical deformity, similar to postulated etiologies regarding the development of CMT. Congenital torticollis may also be associated with congenital abnormalities in the vertebral column, spinal cord, heart, and genitourinary tract.2
Torticollis is a presenting symptom, and many causes have been identified.17 As treatment can be time-sensitive, it is wise to thoroughly evaluate patients for all causes to establish an accurate diagnosis as promptly as possible. CMT is the most common form, but there are several other causes of congenital torticollis.
When assessing a patient presenting with torticollis, radiographic imaging is typically performed to rule out structural abnormalities of the bony vertebral column. Klippel-Feil syndrome, a rare disorder characterized by two or more fused vertebrae, is one such congenital bony disorder to rule out. Though the actual incidence is currently unknown, the vast majority of literature approximates it to be an incidence of around 1 in 42,000 live births. In comparison, recent studies have described it as more prevalent at around 1 in 172 live births.18 It can be characterized by a classic triad of a short neck, low posterior hairline, limited flexibility in the face, neck, or upper body, pain in the head, neck, or back, and hearing loss.19
Some other vertebral anomalies important to rule out include congenital occipitocervical synostosis and basilar impression/basilar invagination. It is reported that there can be craniofacial asymmetry and torticollis in up to 70% of patients with basilar impressions.20 Due to the truncation and misplacement of spinal segments, torticollis may be a natural protective sequela and is often reversible following stabilization of the craniovertebral junction. The goals of surgical management include decompression of the foramen magnum, stabilization and alignment of the craniovertebral junction, and restoration of cerebrospinal fluid flow.20
Further evaluation is warranted when abnormalities regarding the vertebral column are ruled out radiographically and torticollis is associated with an abnormal neurologic exam.
ASSESSMENT OF CONGENITAL TORTICOLLIS
Physical examination for a patient presenting with torticollis should focus on abnormalities or asymmetry related to the skull, neck, sternocleidomastoid, and shoulder while concurrently assessing for neurologic, auditory, and visual function. Visual tests include eye alignment, red reflex, pupillary reaction to light, and ability to fixate on objects.21 Any visual deficits should prompt referral to an ophthalmologist to assess for potential ocular torticollis. As discussed, physical exam findings may display a limited passive range of motion or palpable fusiform mass (~50% of the time) in the sternocleidomastoid mass type of CMT within the inferior portion of the muscle. The mass will typically exhibit the most growth within the first month of life and subsequently regresses until around six months, likely due to hematoma growth and replacement by fibrous tissue.14 However, if there is no palpable “tumor,” then postural torticollis could be considered. In this most benign form of CMT, there is no mass or tightness of the sternocleidomastoid muscle, and instead, a more abrupt, short-lived, and self-limiting picture is seen.14
Imaging is proven to be valuable for diagnosing torticollis. Ultrasound, radiographs, Computer Tomography (CT) scans, and magnetic resonance imaging (MRI) effectively identify the underlying cause.2,22
If left untreated, congenital torticollis can lead to various long-term sequelae. Some well-described long-term complications are persistent head tilt, cranial deformation, and asymmetry of the face due to uneven growth of the head and facial bones.4 Craniofacial asymmetry is noticeable, particularly in the case of uneven ears or a misaligned jaw. Long-term consequences of this include compromised cosmesis and temporomandibular joint dysfunction.23 This can then further manifest as secondary changes in shape, such as deformational plagiocephaly, scoliosis, and disruptions in function, such as unilateral breastfeeding and asymmetric hand usage.24 There is an association between CMT and scoliosis, where a prevalence of secondary cervicothoracic scoliosis was found in more than 80% of patients presenting with CMT.25 Furthermore, cervical spinal canal deformities have been found in patients with torticollis, potentially due to the deforming forces caused by the shortened and fibrotic musculature of the neck.26 Another potential long-term complication of congenital torticollis is developmental delays such as delays in crawling and walking and speech and language development.2,4,5,12,14,16 It has been found that there was an increased risk of developmental coordination disorder and attention deficit hyperactivity disorder.27 The motor delays may be caused by a lack of movement and muscle strength in the affected side of the body, which can cause abnormal general movement and become an essential factor in developing other neurodevelopmental disorders.27 Interestingly, there seems to be a developmental delay at 2-6 months that patients can “catch up” to by 12-18 months, but then the delay can be seen or “reappear” at school age.24 This may be seen because developmental delays are more visible during school.
Conservative Management
-
Physical Therapy: Often first-line treatment for congenital torticollis. Outcomes are best when initiated before three months of age.4,17 Programs consistent with cervical stretching, cervical and trunk strengthening, and activities to promote symmetrical management. Physical therapy aims to improve the range of motion, strength, and flexibility of the neck.
-
Caregiver Education: Caregivers of infants with congenital torticollis should be taught how to position their baby in ways that will promote proper head and neck alignment, such as changing the baby’s position frequently, avoiding prolonged use of car seats and other devices that may place increased pressure on the neck, and increased supervised prone play.4 Integrating interventions into the daily routine of the family can help to reduce healthcare costs while also helping to prevent secondary complications.
-
Environmental Modifications: Modifying the environment, such as providing supportive pillows, altering infant positions within the crib/table, and placing toys next to the affected side may encourage turning to the tighter side while helping to alleviate discomfort and promoting proper alignment.4
Non-Operative Methods
-
Medications: Most utilized are anti-spasmodic medication and muscle relaxants, as well as botulinum toxin injections in the event of failed conservative management. Botulinum toxin is thought to act in two different ways: (1) as a block inhibiting the release of acetylcholine and reducing stimulation of the affected sternocleidomastoid and (2) as a neurotoxin leading to controlled muscle atrophy and weakening. Despite being most often utilized in adults, it has been reported to be more than 90% effective in increasing the range of motion in infants.28
-
Orthotics: Wearing an orthotic device, such as a collar or a brace, may help to support the neck and improve alignment. It has been described in the literature as helpful when utilized as a supplement to traditional therapy.17
Operative Management
This is typically indicated for CMT, which does not respond to physiotherapy or other conservative methods. Principles include identification and release of all contractures within the sternocleidomastoid muscle, performing a range of motion exercises before completing the surgery, and physical therapy resumption within 2 weeks of surgery to prevent recurrent contracture formation. There are several options available for surgical management, including simple myotomy, bipolar release of the sternocleidomastoid, open unipolar release and partial resection of sternocleidomastoid, subcutaneous endoscopic tenotomy, subperiosteal lengthening of sternocleidomastoid (SCM), inferior Z-plasty, and even radical resection.7
Evidence is strong that in most cases, earlier intervention in congenital torticollis results in improved patient outcomes and decreased need for extended care.4,5 As such, the physicians and caregivers involved during the newborn period are crucial in their ability to observe for any potential asymmetry and subsequently perform the appropriate evaluative workup. It has been shown that there is improvement in craniofacial asymmetry after surgical management of torticollis, where results were shown to be better when appropriate action was taken prior to 5 years of age.29 This could be because the earlier the intervention, the more growth potential is available to reverse any major asymmetry.7 The extent to which any secondary sequelae may resolve is highly individual and depends on a range of factors, such as the pretreatment severity of torticollis, length of untreated torticollis, age of diagnosis, and treatment effectiveness. Every patient will be unique, and the prognosis for any child will depend on various factors [Figure 2].
AREAS FOR IMPROVEMENT
With its various causes, Torticollis requires a multidisciplinary team to provide coordinated care. Specialists such as pediatricians, orthopedic surgeons, neurologists, ophthalmologists, otolaryngologists, neurosurgeons, and therapists may be involved in the diagnostic process. Streamlining this process is crucial for improving the patient’s quality of life. Zvi et al. provided a clinically relevant assessment tool and management scheme that could assist from differential formation to diagnosis while providing a treatment pathway.14 The article highlights five key features in the clinical history of torticollis: Pain, Intermittent or constant nature, Neurological signs, Congenital or acquired origin, and Head shape. The acronym PINCH conveniently represents these features, which helps ensure a comprehensive approach to differential diagnosis. Painful torticollis may suggest acute atlantoaxial displacement, while intermittent torticollis may be associated with benign paroxysmal torticollis, Sandifer syndrome, or dystonia.
Even more compelling for creating better practices is the evidence from Strenk et al. that initiating timely, optimal access to care while including effective feedback and documentation may improve population outcomes in torticollis by close to 20% over 18 months.30 Articles such as these help provide a primary care provider with a more vigorous initial assessment that could help prevent treatment delay, decrease healthcare costs for the patient, and improve long-term patient outcomes [Figure 3].31
CONCLUSION
This review provides an overview of torticollis, including its causes, diagnoses, and management. Early detection and intervention are crucial for better outcomes, and multidisciplinary care involving healthcare professionals is recommended. Treatment options depend on the specific cause and patient’s condition. Conservative measures are effective for most patients, while surgery is reserved for severe or stubborn cases. Long-term prognosis is generally favorable, but follow-up and ongoing management are essential for optimal outcomes. Further research is needed to explore the causes and optimal treatments, including non-invasive neuromodulation. This review aims to enhance disease understanding, improve patient outcomes, and promote coordination among caregivers and healthcare providers.
Declaration of conflict of interest
The authors do NOT have any potential conflicts of interest for this manuscript.
Declaration of funding
The authors received NO financial support for the preparation, research authorship and publication of this manuscript. d publication of this manuscript
Declaration of ethical approval for study
Not applicable.
Declaration of informed consent
There is no information in the form of names, initials, hospital identification numbers, or photographs) in the submitted manuscript that can be used to identify patients.


_(left)_and_bip.png)

_(left)_and_bip.png)